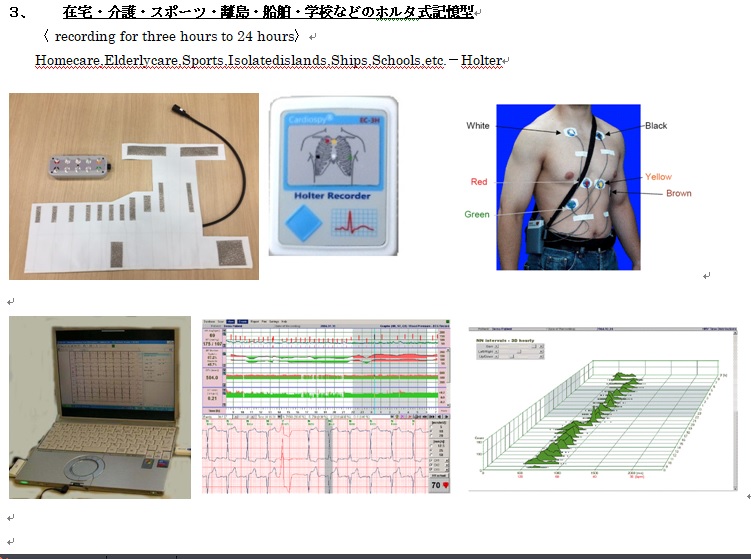
|
|||||||||
| エアロビックの効果 デュナ デュナの実例 ブルーツース ラブテック製品 心電・血圧ホルタ記録器 Labtech products | |||||||||
#冠動脈疾患にはステント治療より #心臓リハビリの運動の方が効果的 8月29日から9月2日のスペイン・バルセロナで開催された #欧州循環器学会のトピックとして注目される発表及び意見が出された。 それは、現在広く行われている血管造影及びバルーンPTCAやステント という診断及び治療方法は、 心臓リハビリなどで行われる運動の方が より患者に優しく、効果的であるとの多数の発表があった。 #ワイヤレス12誘導負荷心電計は、日本でも認可されてご用意されて います。 Exercise beats angioplasty for some heart patients . BARCELONA, Spain . Working up a sweat may be even better than angioplasty for some heart patients, experts say. Studies have shown heart patients benefit from exercise, and some have even shown it works better than surgical procedures. At a meeting of the European Society of Cardiology on Sunday, several experts said doctors should focus moreon persuading their patients to exercise rather than simply doing angioplasties. Angioplasty is the top treatment for people having a heart attack or hospitalized with worsening symptoms. It involves using a tiny balloon to flatten a blockage and propping the heart artery open with a mesh tube called a stent. Most angioplasties are done on a nonemergency basis, to relieve chest pain caused by clogged arteries cutting off the heart's blood supply. " It's difficult to convince people to exercise instead of having an angioplasty, but it works," said Rainer Hambrecht of Klinikum Links der Weser in Bremen, Germany. Hambrecht published a study in 2004 that found that nearly 90 percent of heart patients who rode bikes regularly were free of heart problems one year after they started their exercise regimen. Among patients who had an angioplasty instead, only 70 percent were problem-free after a year. Hambrecht is now conducting a similar trial, which he expects to confirm his initial findings: that for some heart patients, exercise is more effective than a surgical procedure. Other experts agreed that would likely be the case. An angioplasty "only opens up one vessel blockage," said Dr. Christopher Cannon, an associate professor of medicine at Harvard University and spokesman for the American College of Cardiology. He was not linked to Hambrecht's research. " Exercise does a lot more than fixing one little problem." Among other benefits, exercise lowers bad cholesterol while raising good cholesterol, helps the body process sugar better, improves the lining of the blood vessels and gets rid of waste material faster. Exercise also lowers blood pressure and prevents plaque buildup in the arteries. Previous research has estimated one third of heart disease and stroke could be prevented if patients did two-and-a-half hours of brisk walking every week. In the U.S., that would mean 280,000 fewer heart-related deaths every year. Joep Perk, a professor of health sciences at Sweden's Kalmar University and spokesman for the European Society of Cardiology, said two thirds of heart patients in line for an angioplasty could probably get better benefits by regularly working up a sweat. Experts say less than 20 percent of heart patients get the recommended amount of exercise . about 30 minutes of moderate activity five times a week. Perk said doctors who performed angioplasties on their patients without asking them to change their lifestyles were ignoring the fundamental problem. "It would be like getting rid of the most troubled rust spots on a car without doing anything to stop more rust from appearing tomorrow." Still, doctors admitted that persuading patients to exercise instead of simply going in for an angioplasty, which can take less than a day, would be a tough sell. " Most patients want the quick fix," Cannon said. Exercise may improve patients' hearts better than an angioplasty, but it may also take months or even longer for patients to feel the benefits. " It's a lot easier to get your artery fixed than it is to exercise every day." ____ On the Net: http://www.escardio.org |
|||||||||
|
|||||||||
|
|||||||||
|
|||||||||
|
|||||||||
|
|